Prenatal Perspectives Fast Facts: The Zika Virus
Reem S. Abu-Rustum, MD
[email protected]
(Date of Submission 7 February 2016)
With this issue, we introduce to our readers the new “Prenatal Perspectives Fast Facts” which shall address new and emerging topics in prenatal diagnosis. It is by no means a comprehensive review on the subject, yet it aims at highlighting the main points and provides key references for an in depth review of the topic. We choose the Zika Virus as our first topic. We welcome our reader’s suggestions as to future content.
- What is the Zika virus? Zika is an “Arbovirus” that was first discovered in the Zika Valley, Uganda, in 1947 (1).
- Where is it present? Initially, Zika was confined to Africa, Asia and South Pacific. However, there are now reported cases in South America and the USA. The first reported case in the USA was in New York in 2013 (2), and now the most recent outbreak has been in Brazil where the virus is believed to have arrived in 2014 (2).
- How is it transmitted? Zika is transmitted by the Aedes genus, mainly Aedes aegypti mosquito (3). Zika has been shown to be present in human blood, urine, semen and amniotic fluid. It can be transmitted by blood and in-utero (4). Recent reports have also provided evidence that it can be sexually transmitted from an infected male to his partner. It is uncertain if it can be transmitted through urine and saliva (5). There have been no reports of transmission through breast-feeding (4).
- What are its presenting symptoms? In the adults, the disease has mild presenting symptoms including a skin rash, conjunctivitis, arthralgia, fever and headaches that last 2-7 days (3). It has the potential to develop into Guillain-Barre syndrome. In the fetus, it is believed to cause microcephaly.
- How can we test for it? The virus is tested for using PCR, virus isolation from blood and antibody testing (3). However, there is cross reactivity between Zika and dengue, yellow fever and West Nile viruses (3). New York City has just announced that it shall offer free testing to all pregnant women who have travelled to a country with a Zika outbreak (6).
- How is it treated? There is no treatment for Zika’s mild symptoms except for bed rest and supportive care (1).
- How is it transmitted to the fetus? It seems that Zika is transmitted transplacentally and it has been found in amniotic fluid as well as placental tissue (4).
- How can we diagnose prenatal fetal infection? An infected fetus has been shown to have microcephaly, ventriculomegaly, intracranial calcifications as well as orbital calcifications. Though microcephaly may be easier to recognize, it tends to be a later manifestation in case of an inutero fetal infection. Whenever any sonographic abnormalities are detected on routine sonographic evaluation, then fetal Zika virus infection should be suspected in the applicable clinical context (7).
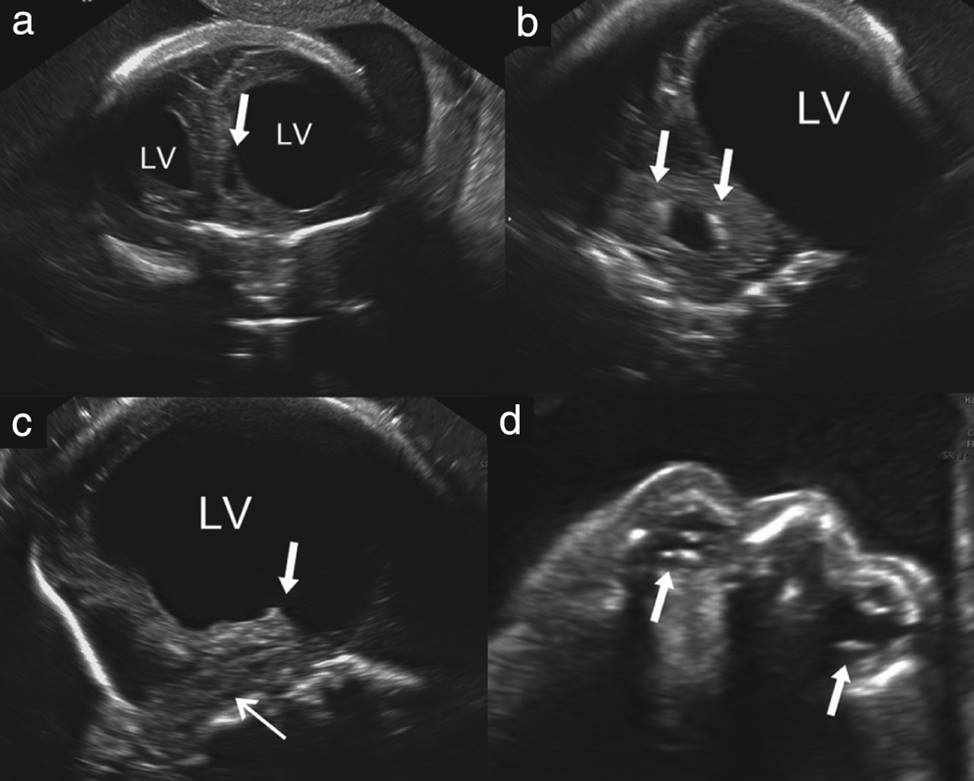
Image and caption reproduced with UOG permission. Oliveira Melo, A. S., Malinger, G., Ximenes, R., Szejnfeld, P. O., Alves Sampaio, S. and Bispo de Filippis, A. M. (2016), Zika virus intrauterine infection causes fetal brain abnormality and microcephaly: tip of the iceberg?. Ultrasound Obstet Gynecol, 47: 6–7. doi: 10.1002/uog.15831
Ultrasound examination in fetus with vertical transmission of Zika virus, resulting in microcephaly. (a) Anterior coronal view shows severe asymmetric ventriculomegaly with cystic formation (arrow). (b) Posterior horn of the lateral ventricle (LV) in coronal view is dilated. Note calcifications in the fourth ventricle (arrows). (c) The thalamus is absent (arrow) and the brainstem and pons are thin and difficult to visualize (sagittal view). (d) Axial view shows calcifications in both eyes (arrows). Note that the proximal eye is very small and lacks normal anatomic landmarks.
- How should we manage at-risk fetuses? Mothers who are at risk, having travelled to endemic areas, or who reside in an affected area, need close sonographic surveillance as per the CDC’s algorithms (8).

Adapted with permission from “Updated Interim CDC Guidance: testing algorithm for a pregnant woman with history of travel to an area with ongoing Zika virus transmission”

Adapted with permission from “Interim CDC Guidance: testing algorithm for a pregnant woman residing in an area with ongoing Zika virus transmission, with or without clinical illness consistent with Zika virus disease”
- How can we prevent it? Currently, there is no vaccine available for Zika. There are global efforts underway to prevent the spread of Zika: from insect repellents, to wearing long sleeves, to encouraging condom use whenever a partner has travelled to an endemic area, to recommending delaying pregnancy. And most recently, “biotech bugs”, which are genetically engineered mosquitos that pass on a lethal gene to their offspring, so that they die before adulthood, are being evaluated for the control of Zika (9). In Australia, where there have been no cases of Zika thus far, mosquitos that have been infected by the “Wolbachia” bacteria are being bred in backyards. Wolbachia prevents the mosquitos (and their offspring) from carrying various pathogens such as Zika. The ultimate aim is to have these mosquitos outnumber the various other Zika-carrying types (10).
References
- NEJM: http://www.nejm.org/doi/full/10.1056/NEJMp1600297
- New York Times: http://www.nytimes.com/2016/02/07/health/zika-virus-brazil-how-it-spread-explained.html?rref=collection%2Fnewseventcollection%2FZika%20Virus&action=click&contentCollection=Health&module=Collection®ion=Marginalia&src=me&version=newsevent&pgtype=article
- WHO: http://www.who.int/csr/disease/zika/en/
- CDC Zika Virus: http://www.cdc.gov/zika/
- New York Times: http://www.nytimes.com/2016/02/06/world/brazil-finds-zika-virus-in-human-urine-and-saliva-but-risk-is-unclear.html?rref=collection%2Fnewseventcollection%2FZika%20Virus
- New York Times: http://www.nytimes.com/2016/02/05/nyregion/new-york-state-to-offer-free-zika-testing-for-pregnant-travelers.html?ribbon-ad-idx=6&rref=collection/newseventcollection/zika-virus
- ISUOG’s Physician Alert: http://onlinelibrary.wiley.com/doi/10.1002/uog.15831/epdf
- CDC Interim Guidelines: http://www.cdc.gov/mmwr/volumes/65/wr/mm6505e2er.htm?s_cid=mm6505e2er.htm_w
- New York Times: http://www.nytimes.com/2016/01/31/business/new-weapon-to-fight-zika-the-mosquito.html?smprod=nytcore-iphone&smid=nytcore-iphone-share
- New York Times: http://www.nytimes.com/2016/02/05/world/australia/zika-virus-australia-mosquito-experiment.html?ribbon-ad-idx=6&rref=collection/newseventcollection/zika-virus
Other Useful Links
- CDC Morbidity and Mortality Weekly: http://www.cdc.gov/mmwr/volumes/65/wr/mm6502e1.htm
- AMA Zika Virus Resource Center: http://www.ama-assn.org/ama/pub/physician-resources/public-health/zika-resource-center.page?&utm_source=BHClistID&utm_medium=BulletinHealthCare&utm_term=020516&utm_content=MorningRounds&utm_campaign=BHCMessageID
- ECDC Zika Virus: http://ecdc.europa.eu/en/healthtopics/zika_virus_infection/
- The Lancet: http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(16)00080-5/abstract
Fast Facts is developed and edited by Reem S. Abu-Rustum, MD. Please send comments and suggestions to
[email protected].